Lesley Wylie

Lesley Wylie is the manager of a dementia specialist home in Bishopton run by the charity Erskine, who have been caring for Scotland’s veterans since 1916. Proud of the relationship-centred culture within the Erskine Park Home, Lesley is motivated to promote care home nursing role as an innovative and developing area of practice.
I started off doing a physics and instrumentation degree – but I got married and moved down south before I completed it. The first job I got there was as a care assistant in a care home and I absolutely loved it – I was really drawn by the deep relationships you quickly formed with the people you cared for. So, I applied to do my nurse training, still working in the care home while doing so.
 After qualifying, I worked in oncology and neurology wards briefly, but I really missed the long-term relationships which you have working in residential care. So, I moved into care home nursing in 2001, and for the last ten years have been working with Erskine. It is a very forward-thinking organisation, Erskine was the first care home environment in Scotland to employ an Advanced Nurse Practitioner and a Dementia Nurse Consultant and, the nurses here are really encouraged and supported to develop their practice.
After qualifying, I worked in oncology and neurology wards briefly, but I really missed the long-term relationships which you have working in residential care. So, I moved into care home nursing in 2001, and for the last ten years have been working with Erskine. It is a very forward-thinking organisation, Erskine was the first care home environment in Scotland to employ an Advanced Nurse Practitioner and a Dementia Nurse Consultant and, the nurses here are really encouraged and supported to develop their practice.
I can’t imagine working anywhere other than in a care home – I just wouldn’t get the same joy and fulfilment out of my job. I am lucky because not only is this a care home, but we are caring for veterans, so for me, you’re ticking two boxes. I have a real passion for caring for our veterans – it is something I really believe in.
I am responsible for all aspects of the day-to-day operations of the home of 40 residents and driving forward quality and standards in the home.
 My role includes the training and supervision of around 80 staff. I have an open-door policy across the home and like to be a visible leader to staff and residents, I like to be involved. Creating a team where everyone supports each other is important to creating an atmosphere in the care home which feels safe and comfortable. It also provides an atmosphere where change is embraced and not only embraced but encouraged so we are constantly improving the care provided to those living here.
My role includes the training and supervision of around 80 staff. I have an open-door policy across the home and like to be a visible leader to staff and residents, I like to be involved. Creating a team where everyone supports each other is important to creating an atmosphere in the care home which feels safe and comfortable. It also provides an atmosphere where change is embraced and not only embraced but encouraged so we are constantly improving the care provided to those living here.
In care home nursing, your drive is to make people’s life worthwhile and meaningful – nothing is too small. Residents can come to my office when they want to. There is one lady who will sit in my office for hours with her colouring books and she’s no longer distressed when she’s doing that.
I also liaise with families, staff and external agencies to actively promote independence for residents and ensure the delivery of quality relationship-centred care. I’m a driven leader always looking for new and innovative practices that are positive for the residents living in the home and develop the staff.
 To see people living with dementia, who had to give up their home to come into a new environment, and watching them feel safe and secure here and grow to have a positive home life is probably the main driver for me. I see my role as a community nurse as ensuring people who are living with dementia are fulfilled and making every moment count in the life they are leading.
To see people living with dementia, who had to give up their home to come into a new environment, and watching them feel safe and secure here and grow to have a positive home life is probably the main driver for me. I see my role as a community nurse as ensuring people who are living with dementia are fulfilled and making every moment count in the life they are leading.
Forming trusting relationships is key in doing that – you need the ability to develop strong relationships, be that with the residents, their relatives or your team.
Absolutely everything I do is about making sure that when the residents leave their homes, they are moving into somewhere that will continue to feel like their own home. It is making sure when they come in here that it doesn’t feel clinical.
 Some of the work we have done most recently at Erskine Park Home is a programme called Art Adventures In Nature, a joing programme with Luminate – Scotland’s creative ageing organisation. Residents used different techniques such as photography, storytelling, sculpture, stone carving and painting to create an outdoor exhibition inspired by nature and it is now on display throughout the beautiful woodland behind the home. It’s very much been a positive experience – the residents and staff go for walks or cycles on the on the adapted bikes in this area and they get to see the work they created.
Some of the work we have done most recently at Erskine Park Home is a programme called Art Adventures In Nature, a joing programme with Luminate – Scotland’s creative ageing organisation. Residents used different techniques such as photography, storytelling, sculpture, stone carving and painting to create an outdoor exhibition inspired by nature and it is now on display throughout the beautiful woodland behind the home. It’s very much been a positive experience – the residents and staff go for walks or cycles on the on the adapted bikes in this area and they get to see the work they created.
 I want to develop the care provided in the home I manage by implementing the practice of Namaste. Joyce Simard, the founder of Namaste, states that “it helps people to live – not just exist – with irreversible dementia like Alzheimer’s disease.”
I want to develop the care provided in the home I manage by implementing the practice of Namaste. Joyce Simard, the founder of Namaste, states that “it helps people to live – not just exist – with irreversible dementia like Alzheimer’s disease.”
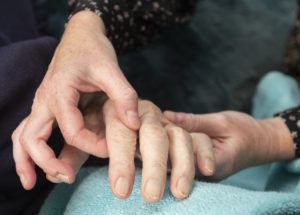
It is a sensory engagement for people who are living with advanced dementia, or those at end of life. It can be helpful, particularly in late dementia, when a person has maybe become really withdrawn, unable to communicate, or take part in the other activities.
We introduced it in my home about two years ago and, as part of the Queen’s Nurse development programme, I am developing and rolling out a training programme in Namaste Care for Erskine with the aim of having it in every home seven days a week. This will mean potentially any of the residents would benefit from Namaste in the later stages of their dementia journey or end of life care. The other three home managers at Erskine and the Director of Care gave their whole-hearted support for my project.
The training involves a two-day programme and will include looking at choreographed touch, how to read aloud to people, how to stage a Namaste area. We do already have a Namaste room in the home and it needs to be set up in a certain way as sound and light and comfort is really important. For people who are end of life we actually take Namaste into their rooms using a mobile trolley.
 The practice is about connection – one technique could be using a playlist for life, a soundtrack of their own songs that have meaning. It’s person-centred – if you don’t know the person you can’t do it effectively for them. You need to understand the person and their preferences and speak with the relatives, it is all about relationship.
The practice is about connection – one technique could be using a playlist for life, a soundtrack of their own songs that have meaning. It’s person-centred – if you don’t know the person you can’t do it effectively for them. You need to understand the person and their preferences and speak with the relatives, it is all about relationship.